Private Medical Dermatology
in Liverpool and Chester: A Handy Guide
by Dr. Thiru, Last Updated on 3 Mar 2026
What’s the Difference Between Aesthetic and Medical Dermatology?
Aesthetic dermatology focuses on skin issues that aren’t inherently harmful but can affect how people feel about their looks. These skin imperfections can stay for years without harming health. Aesthetic care may include non-surgical treatments used in medical dermatology, such as injection of dermal fillers for thin lips, as well as minor surgical procedures like manual removal of skin tags.
What Skin Conditions Does Medical Dermatology Treat?
Medical dermatology handles a wide range of skin problems, including the common disorders listed below.
Acne
Acne happens when hair follicles (pores) clog with oil and dead skin cells, letting bacteria grow and spark inflammation. Hormones, family history, certain medications, and stress can increase risk. Lesions may include whiteheads, blackheads, red pimples, or painful, pus-filled bumps on the face, back, and chest. Acne scars, dark marks, and diminished confidence are possible complications.
Eczema
This inflammatory skin condition involves weakening of the skin’s protective shield, making it more sensitive to irritants and allergens. Contributors may include family history, dry skin, or environmental factors like harsh soaps and weather changes. The skin may be red, dry, itchy, cracked, or oozing, often on the hands, elbows, knees, and face. Without prompt care, eczema can persist and cause skin thickening, infection, and discomfort.
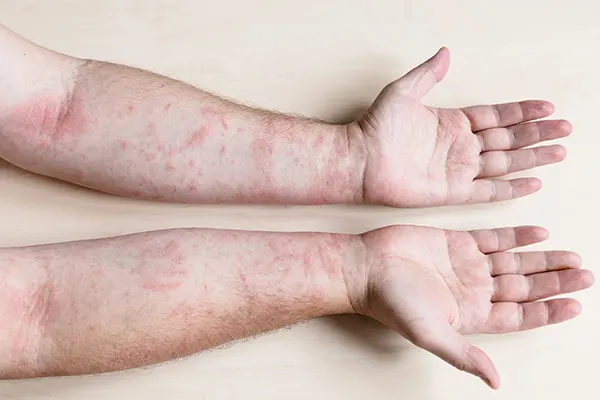
Atopic Dermatitis. This itchy, inflammatory skin disease is a form of eczema that often runs in families
Psoriasis
This immune-driven skin disease accelerates the life cycle of skin cells, causing thick, scaly patches. A family background of psoriasis increases the risk of developing the condition. Stress, infections, smoking, alcohol use, and certain medications can trigger or worsen flares.
Lesions are typically red or pink with silvery-white scales, commonly on the elbows, knees, scalp, and lower back. Untreated psoriasis can cause joint problems, heart disease, and kidney or liver strain.
Rosacea
This recurrent inflammatory skin problem affects facial blood vessels and glands, leading to persistent irritation and redness. Fair skin and family history are risk factors, while sun exposure, alcohol, spicy foods, and stress can start flare-ups.
Common signs include facial redness, visible blood vessels, and small skin lumps that may sometimes contain pus. If left unmanaged, this disorder can cause eye irritation and, in severe cases, permanent skin thickening, especially around the nose.
Skin Infection
Skin infections occur when germs invade the skin, often entering through small cuts or cracks. Close contact with affected individuals, poor hygiene, reduced immunity, and warm, moist environments increase risk. Without treatment, some infections may spread, recur, create permanent scars, or, in severe cases, become life-threatening.
Symptoms vary. Cellulitis, caused by bacteria, produces red, tender, swollen skin. Warts, due to viruses, appear as rough growths. Ringworm, a fungal infection, forms circular, scaly patches. Scabies, resulting from mite infestation, leads to intense itching and small skin bumps typically on creased areas like the palms and gaps between fingers.
Skin Cancer
This condition occurs when skin cells grow uncontrollably, often forming abnormal spots or lumps. Risk factors include fair complexion, excessive sun exposure, family history, and weakened immunity. If not treated immediately, skin cancer can spread to other parts of the body, possibly becoming fatal.
The most frequently seen types are basal cell carcinoma, creating pearly or waxy tumours, and squamous cell carcinoma, which can appear as scaly, red patches. Melanoma, the deadliest form, often begins as a rapidly evolving mole.
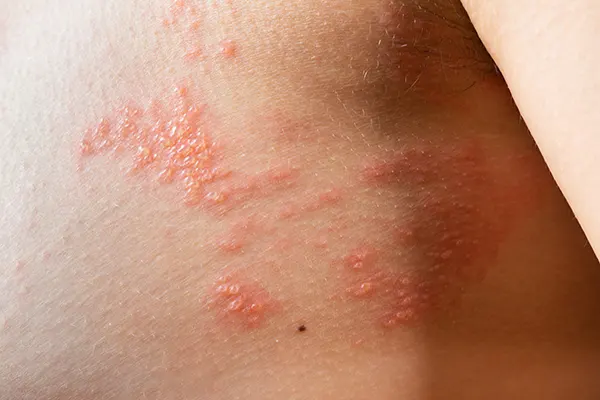
Shingles. This painful, blistering viral rash usually appears in a band-like pattern on one side of the body, often when the immune system is suppressed
Disorders of the Hair and Nails
Hair and nail diseases arise from a wide range of causes, from genetic factors and hormonal shifts to infections, nutritional gaps, immune abnormalities, and cancer. Common signs include brittle nails, hair loss, unusual growth patterns, discolouration, and scalp itchiness. Early detection allows timely, tailored treatments to manage symptoms, support healthy regrowth, and prevent complications.
When Should You Get a Skin Concern Checked?
Most skin problems in otherwise healthy people settle on their own or respond well to basic measures, such as avoiding flare triggers and gentle cleansing. However, you should seek medical care if you have a skin lesion with the following features.
- Sudden onset
- Persistence, recurrence, or progression
- Unresponsiveness to standard skin treatments
- Significant impact on your confidence or daily functioning
- Association with sensory changes, such as pain or numbness
- Widespread involvement
- Unusual colour, shape, texture, or appearance
- Bleeding or persistent itchiness
A consultant dermatologist is the most qualified healthcare professional to examine and treat skin conditions. Their specialised training allows them to identify underlying causes, provide accurate diagnoses, and recommend treatments tailored to your needs. In Liverpool and Chester, you can turn to Specialist Skin Centre, where Dr Thiru manages both common and complex skin disorders.
What Should You Expect from a Dermatology Consultation?
Your dermatologist will cover specific details, such as when the skin issue began, how it behaves, and any accompanying symptoms like itching or pain. You will also be asked about your medical and family history, lifestyle, and any treatments you have tried. These bits of information are essential for understanding your skin problem and determining therapy.
Many skin conditions can be recognised by their appearance alone, but a full skin exam is still recommended at the first visit. It allows your doctor to perform skin cancer screening and establish a baseline record, all conducted in a professional and respectful manner.
Dermatology Consultation at a Private Clinic
Once the exam is complete, your dermatologist will go over their findings with you before deciding on the next step. For some conditions, a suitable skin treatment may be recommended immediately, but others will need further testing.
What Types of Tests Are Done in Medical Dermatology?
A full skin exam is the first and most important part of a dermatology consultation after the physician takes a detailed patient history. As mentioned, many skin issues can be diagnosed at a glance, without needing additional testing. If the initial exam reveals anything that requires closer inspection, the dermatologist may perform other helpful tests during the visit.
Dermatoscopy, often part of a routine mole check, allows the doctor to see fine details of discoloured areas that aren’t visible to the naked eye. A Wood lamp exam uses UV light to reveal infections or pigmentation changes. Mole mapping involves taking pictures of your moles over time to track changes and decide if skin surgery may be necessary.
Some specialised tests may require a separate appointment. A skin biopsy is a diagnostic surgical procedure that helps confirm whether a spot is cancerous. Further work-up may also involve patch testing to identify allergies, microbiological analysis to detect infections, or blood tests to check overall health.
Imaging tests, such as CT, MRI, or ultrasound, can assess deep organ involvement, particularly in tumours and blood vessel abnormalities. Hair and nail analysis helps detect hair and nail health issues.
Many of these testing services are available at Specialist Skin Centre. However, complex diagnostics, such as CT and MRI, require referral to other facilities.
What Kinds of Treatment Does a Medical Dermatology Clinic Offer?
Medical therapies in dermatology usually avoid large cuts into the skin that could noticeably change its appearance or increase scarring risk. Options include skin-applied products, oral medications, and minimally invasive procedures, which are explained below.

Topical Treatment. Steroid cream is being applied to an allergic rash
Topical Therapies
Many complexion problems begin at the surface due to the skin’s crucial role as a protective barrier against the environment. Damage from a wide range of external factors, such as sun exposure, insect bites, pollution, and germs, may be amplified by your immune response.
Mild, localised skin problems that don’t reach deeper tissues can arise from these processes, often treated with topical therapies. You can find these products in the form of creams, ointments, lotions, gels, or solutions. They focus on the problem area and don’t cause issues elsewhere in your body.
However, scattered, recurring, or rapidly spreading skin eruptions often signal underlying conditions, such as severe allergies, infections, or other medical disorders. Treating the root cause is critical in these cases, with skin treatments only having a supportive role.
Oral Medications
Oral treatments are taken by mouth and help manage skin concerns that topical therapies alone can’t control. For example, people with stubborn or severe acne can benefit from the highly effective, vitamin A–derived acne treatment, isotretinoin. Risankizumab targets the immune system to control psoriasis.
Oral medications can reach areas that topical treatments cannot, targeting the underlying causes of skin conditions rather than just the visible symptoms. But since these drugs travel through your body, they may sometimes affect your other organs, particularly your liver and kidneys, where they’re processed or flushed out. Careful supervision by a doctor is essential to ensure your safety while using these medications.
Minimally Invasive Procedures
These non-surgical, dermatologist-led treatments include injections, microneedling, chemical peels, and light-based technologies, such as UV phototherapy and photodynamic therapy. They target skin conditions with little disruption to surrounding tissue.
Minimally invasive procedures may be used alone or combined with topical or oral medications to enhance their effectiveness while reducing the need for higher doses or strengths. For example, phototherapy supports faster or more complete responses in conditions like severe, hard-to-treat psoriasis by delivering UV light directly to affected areas.

Oral Medication. A girl in her late teens is taking an isotretinoin pill for recurrent pimple breakouts
The risks vary by procedure and patient variables. Your skincare specialist carefully considers these factors to ensure the treatment you get is both safe and effective.
Specialist Skin Centre offers an extensive array of medical dermatology services to treat skin, hair, and nail conditions. Learn more by visiting our Medical Dermatology page.
How Can You Benefit from Seeing a Private Dermatologist?
In the UK, including the North West, you can access NHS dermatology services free of charge. The first step is to consult a doctor in general practice—your GP—who may refer you to the nearest hospital dermatology department if you need specialist care. However, routine appointments, such as cases that don’t involve emergencies or skin cancer, typically come with long wait times, usually weeks or months.
In contrast, a private dermatology clinic lets you book appointments directly with a consultant dermatologist, often within days. If you have a sudden breakout, you can be seen and get relief quickly. If you’re dealing with a recurrent skin problem, you can maintain regular care with the same consultant dermatologist. However, you’re responsible for consultation fees.
Private dermatologists have the same training as NHS specialists, and their clinics can perform minor procedures, such as mole removal or biopsies. Here at Specialist Skin Centre, you’ll get the same trusted, scientifically supported treatments, customised to your needs to ensure both safety and effectiveness.
Medical Dermatology: Specialised Care for Skin Conditions Requiring Swift Action
To sum up, medical dermatology is a scientific discipline that addresses skin concerns resulting from underlying health problems. That said, every case demands a quick, personalised solution to avoid potential complications. Importantly, identification and management of underlying conditions are core services at a medical dermatology clinic, with therapies usually avoiding skin surgery.
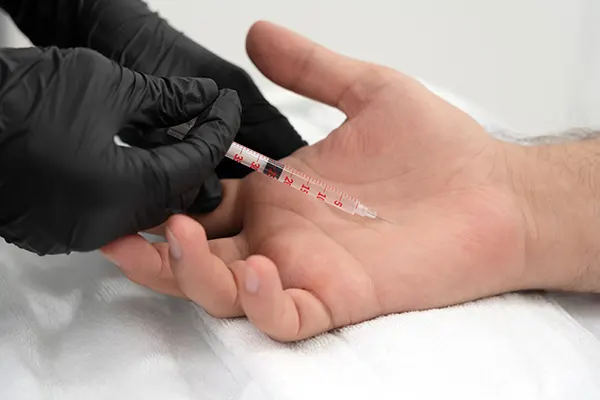
Minimally Invasive Treatment. A medicated solution is being injected into a resistant wart
If you live in Liverpool or Chester, you can access free dermatology care through the NHS, but long waits are typical for non-critical skin concerns. Alternatively, a private dermatology clinic can get you in touch with a consultant dermatologist faster without reducing the quality of care.
Both NHS and private dermatologists hold the same qualifications and adhere to identical professional standards. Private dermatologists provide invaluable support to the NHS by ensuring consistent follow-up, quick access to patient care, and individualised treatment.
In the North West, Specialist Skin Centre has built a solid reputation in medical, aesthetic, and surgical dermatology, thanks to the vast expertise of our consultant, Dr Thiru. Rest assured that, at our clinic, you can get expert help for all skin concerns whenever you need it.
Frequently Asked Questions
Here are some frequently asked questions about skin care and medical treatments:
Looking for deeper answers about medical treatments, results, and aftercare? Our patient questions section covers everything in one place.

